Ce sunt hemoroizii?
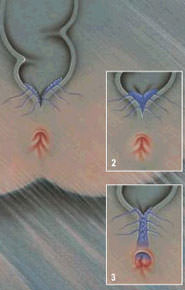 Hemorrhoids are (varicose) vein dilations, occurring inside the anal canal, at a depth of approx. 4-5 cm, through the dilation of small venous pouches caused by constipation, family inheritance or prolonged sitting (office work). You should remember that after their onset, these varicose veins continue to enlarge, considering that, due to their location, they are daily traumatized by defecation. The phenomenon consists of the dilation of the dilation of the cavernous tissue, accompanied by the haemorrhoidal masses prolapsing through the anal canal, their injury leading to post-defecation bleeding, venous stasis and thrombosis, often associated to edema and necrotic phenomena. There are three types of haemorrhoids: internal, originating in the internal plexus, external, originating in the external plexus and combined haemorrhoids.
Hemorrhoids are (varicose) vein dilations, occurring inside the anal canal, at a depth of approx. 4-5 cm, through the dilation of small venous pouches caused by constipation, family inheritance or prolonged sitting (office work). You should remember that after their onset, these varicose veins continue to enlarge, considering that, due to their location, they are daily traumatized by defecation. The phenomenon consists of the dilation of the dilation of the cavernous tissue, accompanied by the haemorrhoidal masses prolapsing through the anal canal, their injury leading to post-defecation bleeding, venous stasis and thrombosis, often associated to edema and necrotic phenomena. There are three types of haemorrhoids: internal, originating in the internal plexus, external, originating in the external plexus and combined haemorrhoids.
Haemorrhoid stages. The presence, moment and the possibility to reduce the haemorrhoidal prolapse help classify the stage of the haemorrhoids and provides therapeutic approach guidance. 1st stage – rectorrhagia (anal bleeding) after defecation, without haemorrhoidal prolapse (haemorrhoids do not come out of the anal canal). 2nd stage – haemorrhage is accompanied by the prolapse (protrusion) of the haemorrhoid masses, which can which can spontaneously reduce in size. 3rd stage – rectorrhagia with haemorrhoidal prolapse, requiring the manual insertion of the haemorrhoids into the anal canal, initially only after defecation and then after efforts that increase intraabdominal pressure. 4th stage – minim effort causes the haemorrhoidal masses to prolapse (protrude through the anus), they often become thrombosed, they are very painful and associated with important life-threatening haemorrhages.
Symptoms of Haemorrhoids
The symptoms of haemorrhoids are anal bleeding, with bright-coloured blood, followed by their prolapse outside the anus, accompanied by anal discharge noticeable on the underwear and by an unpleasant anal pressure sensation, anal pruritus (itching), external haemorrhoidal thromboses. Post-defecation haemorrhages can actually cause anaemia. As haemorrhoids enlarge, they permanently prolapse, the thrombose with edema arises, as well as the throttling of the anal canal, with necrotic tissue modifications. Other symptoms associated to the presence of haemorrhoids are:
- burning sensation;
- swelling (prominences) in the rectal area;
- fistulae, anal abscesses;
- pain during defecation;
- blood in the stool or on the toilet paper;
- inflammation
- pain and discomfort when sitting (driving, office work).
Causes of Haemorrhoids
In the case of people who do not suffer from constipation, quite some years may pass before they are correctly diagnosed as suffering from the haemorrhoidal disease, up to advance stages, if they have no subjective symptoms. However, patients who do suffer from constipation go to the doctor early, because the bleeding worries them.
There are several theories explaining the causes of haemorrhoids, from the infectious etiology (cryptitis, haemorrhoidal phlebitis, colitis) up to neurologic and endocrine conditions. Some authors explain the occurrence of haemorrhoids as a consequence of diet (abuse of spices, alcohol and an unbalanced diet). The occurrence and prolapse of haemorrhoids may be favoured by several factors; hypodynamia, a sedentary lifestyle, obesity, constipation, pregnancy and childbirth, smoking, lifting weights, chronic coughing, abuse of alcohol and spices.
Diagnosis
Haemorrhoids are diagnosed through anamnesis, the patient’s symptoms upon presentation, clinical signs, inspection, examination, videorectoscopy, which helps directly view the rectum. In order to exclude other causes of bleeding, the physician may examine the rectum and the lower area of the colon (sigmoid) through sigmoidoscopy or even examine the whole colon through colonoscopy. Sigmoidoscopy and colonoscopy are diagnosis procedures that exclude the possibility of more severe pathological lesions (colon cancer, polyps, colitis) accompanied by bleeding.
Haemorrhoid Treatment in Laurus Medical Clinics
Haemorrhoid treatment with ointments, suppositories, teas is but an illusion. Even if it alleviates the symptoms and the bleeding stops, the haemorrhoidal disease continues to progress. HEMORRHOIDS DO NOT HEAL BY THEMSELVES or by drug treatment, which only temporarily relieves symptoms.
The minimally invasive outpatient treatment of the haemorrhoidal disease used in Laurus Medical Clinics includes:
- rubber band ligation;
- IR photothermocoagulation;
- radiofrequency ablation;
- monopolar and bipolar coagulation.
Rubber band ligation and IR photothermocoagulation continue to be the golden standard in the treatment of uncomplicated haemorrhoidal disease cases.
Laurus Medical’s proctologists are yearly updated on the medical advancements in the field of proctology, by constantly participating (and by publishing their own results), in the European Coloproctology and Rectal Cancer Congress held each year in Saint Gallen – Switzerland. The event yearly reunites more than 2000 proctologists coming from all over the world, to share their clinical experience. Laurus Medical’s team communications in this scientific event have always been widely appreciated due to the wide and varied cases (2000 to 5000 cases per study) and to the excellent results.
Complications
One of the complications of the haemorrhoidal disease is acute haemorrhoidal thrombosis. Haemorrhoidal thrombosis (a hard-elastic, painful, pea-sized perianal swelling) often is the first manifestation of the haemorrhoidal disease. The acute pain, accompanied by the perianal swelling is what most often sends the patient to the doctor’s practice, being often associated with abundant bleeding. In any stage of the haemorrhoidal thrombosis, the mucous membrane above the thrombose haemorrhoids can erode, causing massive haemorrhage. In most cases, the eroded area is an entrance gate for the infection, progressing towards septic complications (abscess, phlegmon).
Rectorrhagia (anal bleeding) can also be the manifestation of another colon pathology, such as colon neoplasm (colon cancer) or inflammatory diseases. Rectal bleeding is the proof of an injury particularly originating in the lower area of the digestive tract (colon, rectum, anus), but which can also be located in its upper area (duodenal ulcer, for instance) in the case of massive haemorrhages. That is why in Laurus Medical Clinics, in order to make sure that the diagnosis is the correct one, in addition to the rectal examination, we also perform the videoanoscopy, the computed videorectosigmoidoscopy and the colonoscopy if the bleeding source is not identified.