What is Gynecology?
Gynecology is the medical branch specializing in the physiology and treatment of the female genital tract. The Obstetrics & Gynecology specialty aims at maintaining the general health condition of young and mature females, focusing on their physiology and the prevention of specific diseases.
The Obstetrics & Gynecology specialty aims at maintaining the general health condition of young and mature females, focusing on their physiology and the prevention of specific diseases. Obstetrics & Gynecology uses routine examinations and a variety of regularly performed tests, depending on the age and the risk factors. In order to detect possible conditions, we recommend that you make an appointment with your gynaecologist at least once a year. However, if you have problems, immediately contact your gynaecologist. Do not wait until your next visit.
Obstetrics & Gynecology services offered by LaurusMedical clinics:
- Consultation
- Transvaginal Ultrasound
- IUT Fitting
- IUT Removal
- Vaginal discharge collection
The services are available in the following LaurusMedical Network clinics:
Gynecology Medical Articles
Contraception
Female contraception may be achieved in three ways:
- The inhibition of ovulation, which may be obtained through prolonged breastfeeding (regular breastfeeding, with a 98% efficiency rate, unless the menstruation returns in the meantime), oral hormonal contraceptives, , the most frequently used contraception method, determines the suppression of ovulation, being indicated as therapy for dysmenorrhea, menstrual disorders, acne, teratogenic drug therapy and offering an efficiency rate of 0.05 – 0.9 (incidence of undesired pregnancies per 100 cases).
- The inhibition of fertilization is achieved through mechanical means (female condom, vaginal diaphragm), tubal ligation, chemical methods – spermicides, hormonal methods (progesterone-only pill, injectable contraceptives, hormonal implants, vaginal hormonal rings), intrauterine devices (inert plastic intrauterine devices, with or without medicine load – copper, progesterone, meant to prevent the ascension of sperm cells, the fertilization or the implantation), natural family planning methods (behavioural method – coitus interruptus or hormonal method – prolonged lactation), with an efficiency of 4-18 (coitus interruptus) or 9 (fertility calendar method) incidence of undesired pregnancies per 100 cases.
- The inhibition of implantation through hormonal methods or IUDs.
Male contraception is achieved by:
- Inhibition of spermatogenesis
- 2. Inhibition of fertilization , which is achieved through natural family planning methods (behavioral – coitus interruptus, mechanical – – condom, which offers a number of advantages: it is relatively cheap, involves no medical risks, it is efficient if correctly used, does not require a medical examination, protects against sexually transmitted diseases).
- Male Sterilization
Genital Infections
Represent the most frequent condition determining women to make a doctor’s appointment (approx. 1/3 of the patients), even though the vagina is normally protected from the pathogens due to the acidity generated by the Doderlein Bacilli. From amongst the factors increasing the genital infection frequency we mention: early sexual intercourse, multitude of partners, abandonment of mechanic contraception (condom).
In so far as the symptoms are concerned, the patient comes to the medical practice for abundant, fetid vaginal discharge, which sometimes varies in nature during the menstrual period, pruritus, pelvic pain, pain upon the sexual intercourse, pain during urination and frequent urination. All women with the symptoms above should contact a physician to have them investigated. Prior to the gynaecologic examination, the patient must avoid ENDOVAGINAL TOILET and sexual intercourse 48 hours before the visit.
Ovarian Pathology
The ovarian pathology also is asymptomatic, and the suggestive signs only appear when the tumour has enlarged or when there already are complications. The pain may vary in intensity from discomfort upon pressure or lower abdomen fullness. Some of the symptoms are: bloating, intestinal transit disorders, abdomen distension, absence of menstruation (amenorrhea), metrorrhagia (bleeding), urinary disorders or weight loss.
If you have any of these symptoms, contact your gynaecologist for investigations. The treatment differs depending on the ultrasound aspect of the cystic ovarian mass, the patient’s age, the related gynaecological disorders and the severity of the symptoms.
Breast Pathology
The breast pathology is revealed by subjective signs and symptoms, such as mammary tension, discomfort or unilateral/bilateral pain, changes in the profile, shape or teguments, spontaneous/provoked mammary discharge, local inflammation, nipple fissures.
Self-examination is critical for a woman’s health, because it helps discover possible cancers at an early stage. During self-examination, the patient will be able to discover nodular formations at the level of the breasts or nipple discharges.
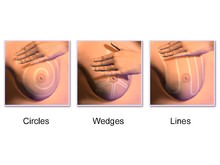
The right self-examination steps:
1. Sit in front of a mirror with your top off. Raise the arm opposite the breast you want to examine above your head. “The main warning sign is the presence of a 1cm nodule in the mammary gland structure. In the case of larger masses, we can no longer speak of incipient cancers, and smaller masses cannot be identified by palpation, but only through mammography. To this end, the breast must not be palpated between two fingers, but you must, instead, press onto the thorax with the tips of fingers 2-5, in small circular movements. Start the examination from the outside of the breast. Do not apply excessive pressure above the breast, but do not palpate it superficially either, because, in this case, you might omit the profound areas of the mammary gland. Make sure you apply the same circular movements to palpate the whose surface of the breast.
2. Then, continue to palpate, using the same circular movements, the area between the armpit and the breast and the armpit area, to identify the possible armpit nodule size changes.
3. Carefully observe the breast to identify possible colour changes in the skin or surface vessels.
4. Look for the possible breast lesions and ulcerations, outgrowths, nipple position or shape changes, changes in the size or symmetry of the breasts.
5. Notice possible nipple discharges or bleeding.
6. Put your arm down and let it hang on the side of your body. Resume the breast palpation in this position.