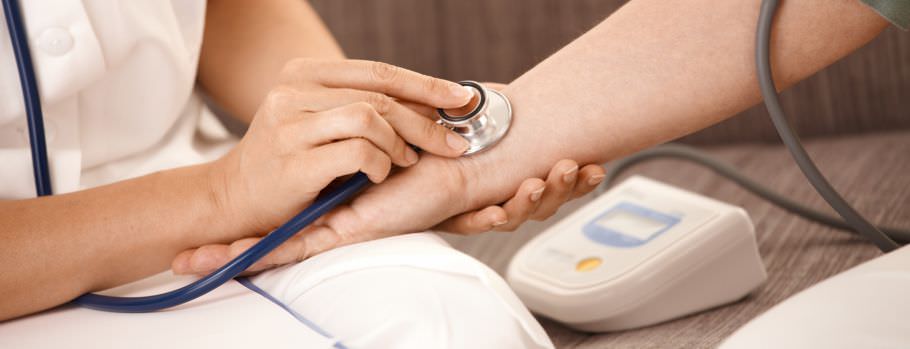
Hypertension continues to be a major public health problem, as it affects a quarter of the adult population in developed countries. There is a direct relation between hypertension and the risk of developing the cardiovascular disease (ischemic cardiomyopathy, myocardial infarction), as well as
the cerebrovascular disease (stroke). The anti-hypertension treatment has been shown to reduce the myocardial infarction risk by an average of 20-25% and the stroke accident risk by 35-40%, on the average. For a long time, the hypertension management guidelines almost exclusively focused on correcting the blood pressure values, but over the past years, the hypertensive patients’ treatment focuses on the assessment of the global cardiovascular risk.
What Are the Cardiovascular Risk Factors?
Or, in other words, what are the conditions associated to a higher cardiovascular disease risk? The family of risk factors was classified into several categories, but the notion of therapeutic intervention or lifestyle change alterable or inalterable risk factors is the most important one for the patient.
The inalterable risk factors are:
- age (the risk is higher after the age of 55 in men and 65 in women)
- the hereditary factor (parents with cardiovascular disease at relatively young ages, below the age of 55 for the father and of 65 for the mother)
- gender (the initial risk is higher in men, but after the menopause, the risk becomes equal, actually becoming higher in women after the age of 75)
The alterable risk factors are:
- smoking
- hypertension
- hypercholesterolemia
- dyslipidemia
- obesity
- diabetes mellitus
- sedentary lifestyle
As you may notice, many of the alterable risk factors are easy to identify and their manager or even correction supposes the joint effort of the physician and patient. The pathway from isolated or even aggregated risk factors to the onset of the cardiovascular disease (the onset of the disease as such) goes through an often asymptomatic stage, which the patient does not notice, known as the subclinical target organ damage period. So, in addition to the cardiovascular risk factors mentioned above, of uttermost importance is the identification of this subclinical damage period, a “silent” disease period, well tolerated by the patient, but with a high reversibility potential, if identified in due time and an efficient treatment scheme is applied. The focus on this stage through the recommendation of specific and individualized therapeutic measures may prevent progression towards the cardiovascular disease stage and, by way of consequence, may influence prognosis.
What are the target organs on which one should focus when assessing a hypertensive patient?
One of the target organs is the heart, and the subclinical damage sign is the presence of the left ventricle atrophy. This heart chamber, the left ventricle, is one of the four chambers of the heart, each with a different role in the pumping functions (pushing the blood column in the rest of the body), as well as in the relaxation function (blood filling). The thickening of the left ventricle walls (LV hypertrophy) may lead in time to cardiac failure.
Another facet of the subclinical damage of an organ is vascular damage, regardless of whether we are speaking about the cerebral or the peripheral lower limb arteries. The monitoring of the renal function also is very important.
Do we currently hold the tools to cast a light on all these actors playing an important role in the cardiovascular risk stratification? Laboratory investigation are a very important tool in diagnosing he traditional cardiovascular risk factors, i.e. a lipidogram with the determination of the total serum cholesterol and of the LDL and HDL cholesterol fractions. The associated diabetes is highlighted through laboratory tests: fasting plasma glucose, glycosylated hemoglobin, glucose tolerance test, while the determination of the BMI (body mass index) provides information on obesity. The renal dysfunction indicators are the serum creatinine, uric acid and glomerular filtration rate determinations.
Imagery investigations are very useful to complete the target organ damage balance. Thus, the echocardiography and the electrocardiogram (EKG) assess the presence of the ventricular hypertrophy (the thickening of the hear walls), as well as other structural (valvulopathies) or functional abnormalities of the heart. In so far as vascular damage is concerned, the Doppler ultrasound at the level of the carotids is very useful, because it provides information on the thickening of the artery walls caused by atherosclerosis – IMT (intima–media thickness), as well as on the development of atheroma plaques. Similar determinations may be performed at the level of the lower limb peripheral arteries. Another vascular damage marker is the measurement of the ankle-brachial index, which can be easily determined by comparing the blood pressure value at the level of the arm with the one measured at the level of the lower limb.
Hence, the early identification of the cardiovascular risk and the determination of the subclinical target body damage are very critical in order to be able to use the entire therapeutic arsenal for the prevention of the irreversible onset of the cardiovascular disease. The prevention-prophylaxis of the disease supposes the joint efforts of two key actors – the physician and the patient – and a clearly set goal: to keep the patient away from the disease and its unpleasant consequences for as long as possible.
For details on the investigations performed within Laurus Medical Bucharest, please access the Cardiology or the Internal Medicine page.