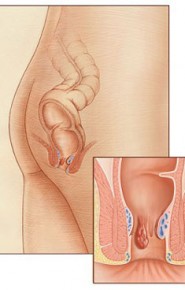
 Because haemorrhoid symptoms are similar to those of an anal fissure, a fistula or an anal abscess, it is very important that the diagnosis be set by a proctologist. However, most people treat haemorrhoids with OTC medication and without previously discussing the matter with the physician. Rectal bleeding, regardless of their cause, must be investigated by a physician. In order to diagnose haemorrhoids, the physician must check the anal area. The physician may also perform a digital rectal exam (DRE) using a sterile glove and lubricant. This exam might be unpleasant if the patient suffers from external haemorrhoids, but it is, however, useful to set a correct diagnosis.
Because haemorrhoid symptoms are similar to those of an anal fissure, a fistula or an anal abscess, it is very important that the diagnosis be set by a proctologist. However, most people treat haemorrhoids with OTC medication and without previously discussing the matter with the physician. Rectal bleeding, regardless of their cause, must be investigated by a physician. In order to diagnose haemorrhoids, the physician must check the anal area. The physician may also perform a digital rectal exam (DRE) using a sterile glove and lubricant. This exam might be unpleasant if the patient suffers from external haemorrhoids, but it is, however, useful to set a correct diagnosis.
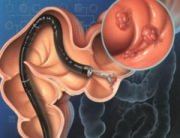
In some cases, more detailed examination might impose the use of an anoscope. The anoscope is a cylindrical medical instrument, equipped with an optical system, which helps view internal haemorrhoids when placed inside the rectum.
Symptoms that may help diagnose haemorrhoids:
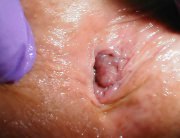
Touch the anal area to identify the presence of a bump (prominence, outgrowth). A round palpable protrusion may be present in the anal canal area, in the case of prolapsed or external haemorrhoids. Prolapsed haemorrhoids are soft and they can be manually pushed into the rectum – this method can temporarily prevent the aggravation of the problem. In the case of external haemorrhoids, the bump is larger and more sensitive to the touch – in this case, haemorrhoids cannot be manually inserted into the rectum to alleviate symptoms. Medical follow-up is recommended in case external haemorrhoids are inflamed and painful.
Unpainful anal bleeding is a common external haemorrhoid symptom and it can also be encountered in some internal haemorrhoid cases. The blood may be present in the faeces, on the underwear, or in the toilet bowl.
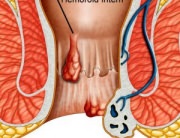
Anal pruritus is a prolapsed haemorrhoid symptom. The pressure in the anal area can cause the internal haemorrhoids to exit the anal canal, causing prolapsed haemorrhoids. This prolapse outside the anal canal causes mucus secretions and the wetting of the skin in the anal area. This continuous wetting, accompanied by the prolapsing of the haemorrhoid upon defecation leads to the anal pruritus.
Skin irritation. Prolapsed haemorrhoids cause the anal area to be continuously wet, which leads to the anal pruritus and, implicitly, to the irritation of the anal area skin, especially if the patient scratches. Try and avoid scratching to prevent further complications.
Post-defecation Discomfort. The incomplete defecation sensation is a common syndrome in the case of haemorrhoids. This sensation is even more unpleasant if the haemorrhoids are inflamed or large.
The Presence of Pain. In the case of internal haemorrhoids, the pain is not very severe, except for prolapsed haemorrhoids. This tissue that prolapses outside the anal canal can very easily become inflamed because of the constant friction exerted onto its surface by the anal sphincter muscles. This contraction of the muscles causes pain, which can be severe in the case of strangled haemorrhoids – in which case the blood flow to the haemorrhoid is interrupted. The immediate medical treatment might be mandatory in order to remedy the problem. Pain is a very common symptom in external haemorrhoids. As the outgrowths form around the anus, the blood is blocked in the prolapsed tissue, leading to the formation of blood clots and thrombosed piles. The friction in the anal area causes the thrombosed external haemorrhoids to swell and inflame, producing severe pain. Emergency medical treatment may be mandatory in this case as well.
Tips and warnings:
Even though most haemorrhoid cases are easy to treat, it is indicated that you address a proctologist in case you have haemorrhoidal disease symptoms. Eat fibre-rich foods and drink plenty of water – these are simple methods to prevent haemorrhoids. If you feel the defecation sensation, do not postpone the elimination of the stool. If the defecation sensation disappear, the stool becomes dry and harder to eliminate, which means that you need to apply more pressure to expel it. This pressure applied onto the blood vessels and the anal area tissues can cause haemorrhoids. Exercise daily. Walking or running helps stimulate the intestinal transit, which, in its turn, helps prevent haemorrhoids.