Patient information on the risks associated to proctological disorders. The latest proctology news, new diagnosis and treatment methods.
External Haemorrhoids
External haemorrhoids may occur as a consequence of the increase of the pressure exerted on the external haemorrhoid veins. When these veins, located around the anus, are swollen and inflamed, there may be symptoms such as pruritus in the anal area, bleeding and pain.
There are a number of risk factors leading to the onset of such symptoms. For instance, pregnancy, obesity and hepatic cirrhosis are some of the causes that may lead to the increase of the pressure on the external haemorrhoid veins.
Treatment options include diet changes, methods to adjust the intestinal transit or surgical intervention. The term haemorrhoids refers to the situation in which the veins located in the anal and lower rectum areas are swollen and inflamed.
Internal and External Haemorrhoid Pictures
Currently pictures of haemorrhoid prolapse, internal haemorrhoids, external haemorrhoids, bleeding haemorrhoids, thrombosed external haemorrhoids, classical haemorrhoids and their typical aspect, small external haemorrhoids are available, as well as pictures depicting the way in which haemorrhoids might change aspect depending on the clinical evolution of the disease. The following haemorrhoid pictures are not meant as a replacement for the proper medical diagnosis and treatment of haemorrhoids.
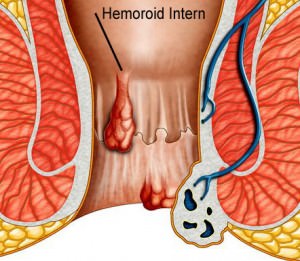
Internal Haemorrhoids
Internal Haemorrhoids may occur as a consequence of the increase of the pressure exerted on the internal haemorrhoid veins. This pressure increase leads to the onset of some symptoms, such as anal discomfort or the presence of bright red blood on the toilet paper (rectorrhagia).
The factors that may lead to the development of this condition include: stool movement straining (defecation straining), obesity or a diet rich in fats and poor in fibres. The treatment strategy involves dietary changes and other ways of adjusting the intestinal transit. If these changes to not relieve the symptoms, the treatment of the haemorrhoidal disease through modern, non-surgical methods is recommended, and in very advanced cases, the surgical intervention is advised.
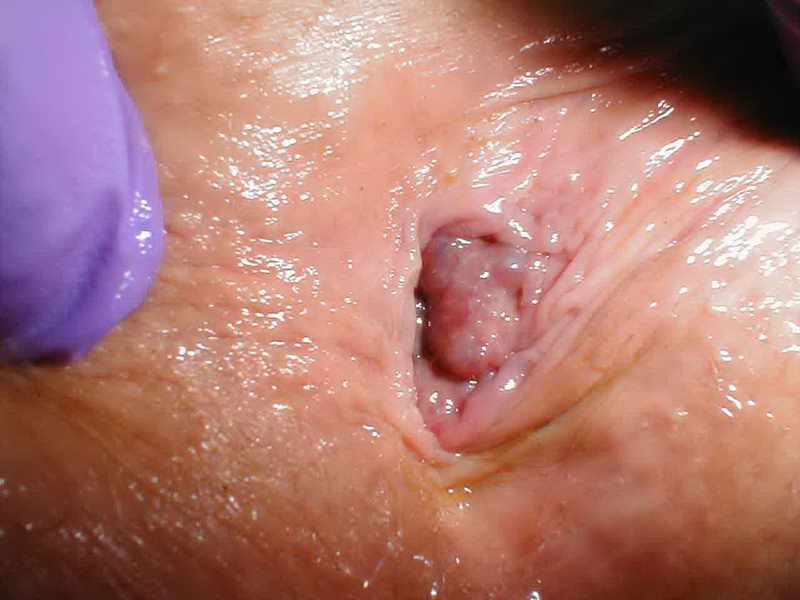
Genital Warts and Condyloma Acuminatum
Genital Warts are the clinical manifestation of an active infection of the male and female genital, perigenital and perianal region skin and mucous membrane, with certain types of human papillomavirus (HPV). The disease is both sexually and non-sexually transmitted (infected hands, iatrogenic, prenatal or perinatal transmission in children). The infection is very contagious and it is frequently associated to other sexually transmitted diseases (syphilis, HIV, etc.), which imposes the performance of the respective tests. In some countries, it is regarded as the most frequently encountered sexually transmitted disease. It should be mentioned that it could become malignant.
The histopathological examination of genital warts:
Only indicated in the cases that do not respond to or worsen during therapy (possible dysplasia), in the case of pigmented, infiltrated injuries or in the case of an uncertain diagnosis.
Haemorrhoid Treatment
medical haemorrhoid treatment supposes the attenuation of the acute haemorrhoid symptoms, especially very acute pain. Doctors recommend a fluid- and fibre-rich diet. Eating proper quantities of fibres and drinking 6-8 glasses of liquid a day (other than alcohol) will help obtain a softer and more consistent stools. A smooth stool facilitates bowel emptying and helps stabilize the pressure on the haemorrhoids caused by constipation. The elimination of constipation also prevents the onset of haemorrhoids. Fruit, vegetables and all cereals are excellent sources of fibre.